Decisions. Some are easy to make, others may come with a bit of challenge. Either way, we all make them daily. Whether it’s choosing to have coffee or tea in the morning, allotting time in your schedule to exercise, deciding how you will budget your summer vacation, or which career field you desire, decisions are a constant. But how often do we realize that each decision made is influenced by the relationships we’ve built over time, and the cultural and physical environment we live in? In public health, the factors that influence behavioral health are outlined in the Social Ecological Model. This theory states one’s behavior is influenced by five over-arching themes: Individual, Interpersonal, Organizational, Community, and Structures and Systems as displayed below.
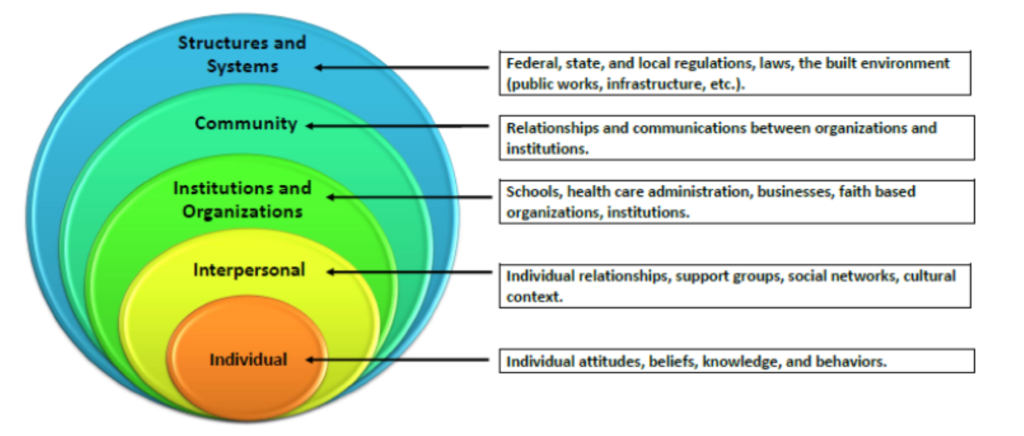
Source: Centers for Disease Control and Prevention, Health Equity Resource for State Practitioners Addressing Obesity Disparities, Health Equity Resource Toolkit for State Practitioners Addressing Obesity Disparities (cdc.gov). December 8, 2017
These factors influence our daily decisions, and ultimately influence our health. As we live through a pandemic, many Americans are faced with the decision to receive a COVID-19 vaccine. Whether the choice is to have it administered or not, the final decision can be influenced by:
- Our personal beliefs (Individual)
- Whether trusted family members or friends have chosen to take it (Interpersonal)
- The work environment we encounter as teachers, nurses, physicians, or other fields (institutions and Organizations)
- Advocacy from the organizations we’re a part of (Community), or
- Our confidence and trust in the federal government may (Structures and Systems)
We would be remiss to discuss the decision to receive a COVID-19 vaccine without acknowledging the minority communities of color that lack trust in the vaccine’s protection. Our country’s history (The U.S. Public Health Service Syphilis Study at Tuskegee (4), the Immortal Life of Henrietta Lacks (3), among other examples) has led to medical mistrust in many black, indigenous and people of color communities. That history makes it quite clear how medical mistrust can spread through generations. This has often led to avoiding doctor visits, not participating in medical trials that can advance scientific research, or even choosing not to receive the COVID-19 vaccine. These decisions can be easily influenced by the factors within the Social Ecological Model. While we, the public health community, must take part in acknowledging this challenge, it is important to advocate and educate through a culturally competent lens to regain the trust in these communities.
Unfortunately, COVID-19 data demonstrate minority communities of color are dying disproportionately at higher rates than other groups of society (1). We also know these communities are susceptible to vulnerable health outcomes. The prevalence of heart disease, hypertension, diabetes, and other health conditions increase the risk for COVID-19 (2). Due to these underlying disparities, many public health organizations and world-renowned celebrities have taken on the responsibility to host forums or filmed conversations with expert scientists and physicians who were part of the creation and trials of the vaccine. Whether through TV or social media, these opportunities not only educate them, but also their target audience and those who are influenced by them. This method of advocacy has been effective, as it can cause paradigm shifts in those who were against receiving the COVID-19 vaccine. Though this is a decision to protect themselves, their families, and members of their community, it is also a way to bridge the gap of trust in scientific studies and medical guidelines.
Through our day-to-day lives, we may not think twice about what influences our decisions, however large or small the role, but those influences can affect our health outcomes. Using this behavioral approach can have an impact in understanding communities we may have little knowledge of. This not only advances public health research and implementation, but it can improve the overall health of the population.
– Astra Watts, Health Communications Specialist II
References
- Centers for Disease Control and Prevention. COVID-19 Racial and Ethnic Health Disparities. 10 December 2020.
- Medical Conditions. 29 March 2021.
- Johns Hopkins Medicine. The Immortal Life of Henrietta Lacks. n.d.
- Tuskegee University. About the USPHS Syphilis Study. n.d.